Introduction
The veteran population is aging rapidly with higher rates of disability compared to non-veterans. The number of veterans age 85 and older is projected to increase by 38% from FY2019 to FY2039, and over 40% of veterans age 65 and older have at least one disability compared to 32% of their non-veteran peers.
A large percentage of older adults over 50 have healthcare coverage through a military-based insurance payer (56.2% total through Tricare, a health insurance program for active-duty military, retirees, and their families made up of 19.6% age 50-65 and 36.6% age 65+, and 74% through the Veterans Health Administration (VHA), the largest integrated health system in the U.S. made up of 22.5% age 50-64 and 51.9% age 65+). Studies of military-based healthcare demonstrate that it outperforms or matches non-military care in most categories, including quality, safety, access, and patient experience. Home and community-based services (HCBS) and mental health services, however, are two areas where military-based healthcare coverage lags behind, particularly for veterans age 65 and older. Two West Health data sources highlight these challenges.
Unmet Need for HCBS Among Older Veterans
Among veterans age 65 and older enrolled in the VHA, 11.5% use HCBS. Veterans who are female, Black, or diagnosed with dementia are more likely to use HCBS, while veterans residing in rural areas are less likely. However, these numbers do not reflect veterans who need HCBS but cannot or do not access it. One study found that 32.3% of veterans with both Activities of Daily Living (ADL) and Instrumental Activities of Daily Living (IADL) limitations reported an unmet need for HCBS.
Underutilization of Mental Health Services Among Older Veterans
Similarly, nearly 1 in 5 older veterans enrolled in VHA services have confirmed mental health diagnoses, and another 26% have documented mental health concerns without a formal diagnosis in their health record. According to data from the West Health Mosaic National Aging Readiness dashboard, 33.2% of women and 30.1% of men age 60 and older with military-based health insurance reported that their mental health was “not good” for 14 or more days of the past month; moreover, 20.9% of women and 23.2% of men in this group have received a diagnosis of depressive disorder from a health professional. Despite higher rates of mental health diagnoses, including post-traumatic stress disorder, older veterans with recently diagnosed depression significantly underuse mental health services, and older veterans in general are less likely to seek mental health services.
Reasons for Unmet HCBS and Mental Health Needs Among Older Veterans
There are a multitude of reasons for this unmet need for HCBS and underutilization of mental health services among older veterans, including systems and cultural barriers.
System-Level Barriers
Older veterans face a variety of system-level barriers that limit their access to HCBS and mental health services. Budgetary constraints and policies limiting HCBS eligibility, inadequate staffing, and provider time constraints are a few of the frequently cited barriers.
According to the Home- and Community-Based Service Use Among Veterans: The National Landscape article in the Journal of the American Geriatrics Society, budgetary pressures at VHA medical centers may contribute to the unmet HCBS needs among older veterans, “forcing tradeoffs between lowering the intensity of care (e.g., hours of care) or type of care provided to increase the extensive margin (e.g., number of people served).” Another way HCBS spending is suppressed by the VHA is by limiting HCBS eligibility to those with a “service-connected disability” (an injury, illness, or disability that was incurred during service in the military). The rate of service-connected disabilities among veterans age 65 and older is much lower than among veterans under 65. One reason is that the policy requiring a service-connected disability for HCBS eligibility did not start until 1944, so many World War II and Korean War-era veterans never received a service-connected disability rating and are unlikely to get one now, limiting their access to HCBS. Veterans are significantly more likely to have a disability that is non-service connected, but these disabilities do not qualify them for VA-funded HCBS. In 2022, about 5.4 million veterans received compensation benefits because of a service-connected disability costing more than $112 billion. Expanding HCBS access to older veterans without a service-connected disability rating would likely add to budgetary pressures and increase costs at a rate that is unsustainable at currently funded departmental levels. A lack of time was also identified as a system-level barrier to HCBS access for older veterans in a study involving family caregivers of veterans.
System-level barriers to accessing mental health services for older veterans are equally challenging. A 2022 study of VHA mental health providers found that inadequate staffing and lack of time to address common barriers to treatment were perceived by providers as highly significant barriers to serving older veterans with dementia.
Cultural Barriers
Even if older veterans can access HCBS and mental health services, many are reluctant to do so because of strongly held military values and beliefs that can be interpreted as stigmatizing seeking and receiving help. It can take a significant amount of effort for a veteran to ask for help because of how they have been trained. Military culture values toughness, resilience, and mission over self, leading some veterans to view seeking help, especially for one’s own functional or mental health, as a sign of weakness.
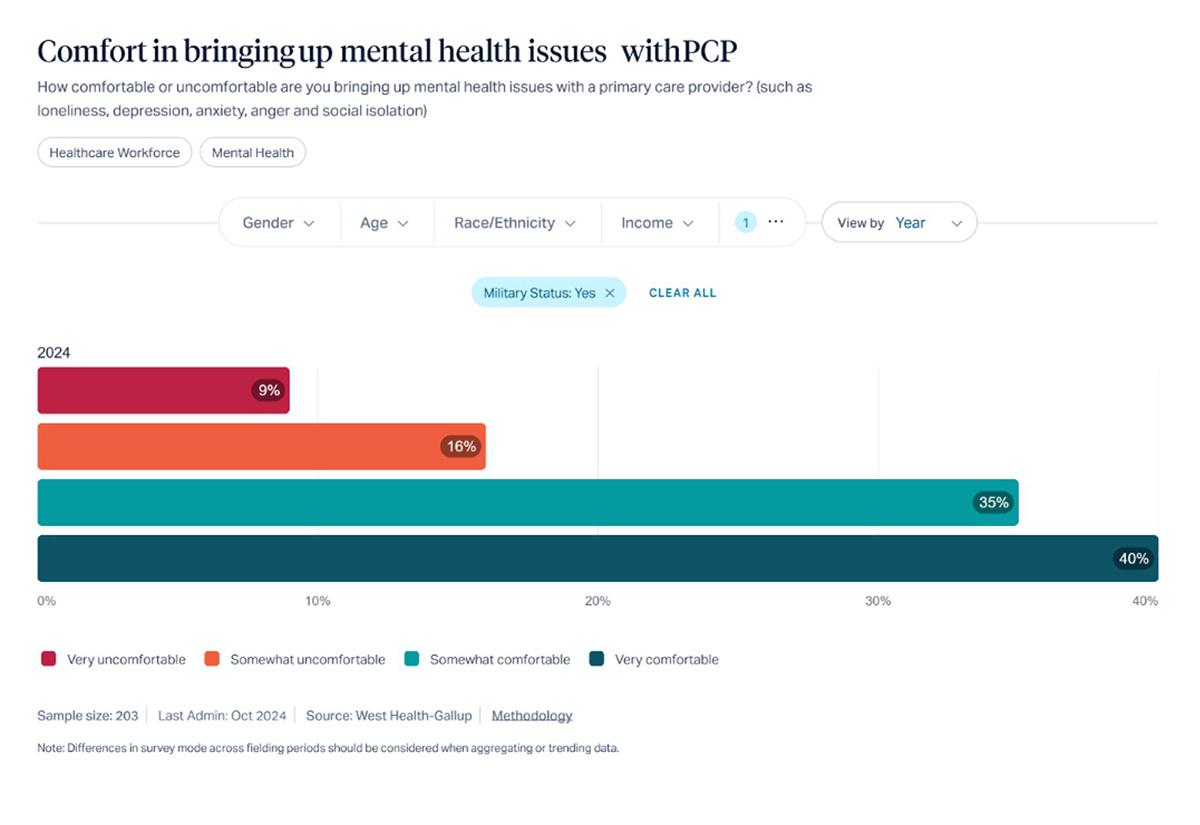
Data from the West Health-Gallup Center for Healthcare in America’s inaugural study, State of the States 2025: Insights on Healthcare in America, illustrates the impact of military culture on help-seeking behaviors among older veterans. Among, 89% indicated there was never a time when they wanted to talk to a healthcare professional about their mental health but were unable to. However, 25% reported being very or somewhat uncomfortable, raising mental health issues with a primary care provider.
Conclusion
Military-based healthcare exceeds quality in many areas, but unmet needs among older veterans in the areas of HCBS and mental health remain. Systems and cultural barriers contribute to this gap. Some of the barriers identified include budgetary constraints, policies limiting HCBS eligibility, inadequate staffing, provider time constraints, and specific military values and beliefs, but ongoing research is needed and more work needs to be done to ensure older veterans get the care they need and deserve.