The Growing Challenge of Food Access for Older Adults
Food insecurity affects millions of older adults in the United States and is becoming more common as the costs of food, healthcare, and housing continue to rise. Limited or fixed incomes, health-related expenses, and access barriers make it difficult for many older adults to maintain consistent access to nutritious food, contributing to poorer health outcomes across communities.
January 22, 2026Food insecurity is a problem that impacts Americans young and old. In 2023, nearly 13% of adults age 50 to 59 and more than 9% of adults age 60 and older experienced food insecurity — an increase from prior years. The U.S. Department of Agriculture (USDA) groups food insecurity into two categories: (1) low food security, defined as reduced quality, variety, or desirability of food, with little or no reduced intake; and (2) very low food security, which involves disrupted and reduced food intake. Some households experience marginal food security, which, although not officially classified as food insecurity, is characterized by anxiety about having enough food available. Recent data show that 84% of adults are somewhat or extremely concerned about the cost of food.
Access to healthy, affordable food is important for maintaining good health and managing chronic conditions. Any level of food insecurity, even marginal food security, is significantly associated with a higher risk of premature mortality and a shorter life expectancy compared with full food security. Among adults age 60 or older who reported experiencing food insecurity, nearly 52% described their health as fair or poor, while only 18% reported being in very good or excellent health. These poor health outcomes lead to more costly health care use, including increased emergency department visits, hospitalizations, and nursing home stays, with an estimated $130 to $160 billion in related costs to the health care system each year.
Factors Shaping Food Insecurity in Older Age
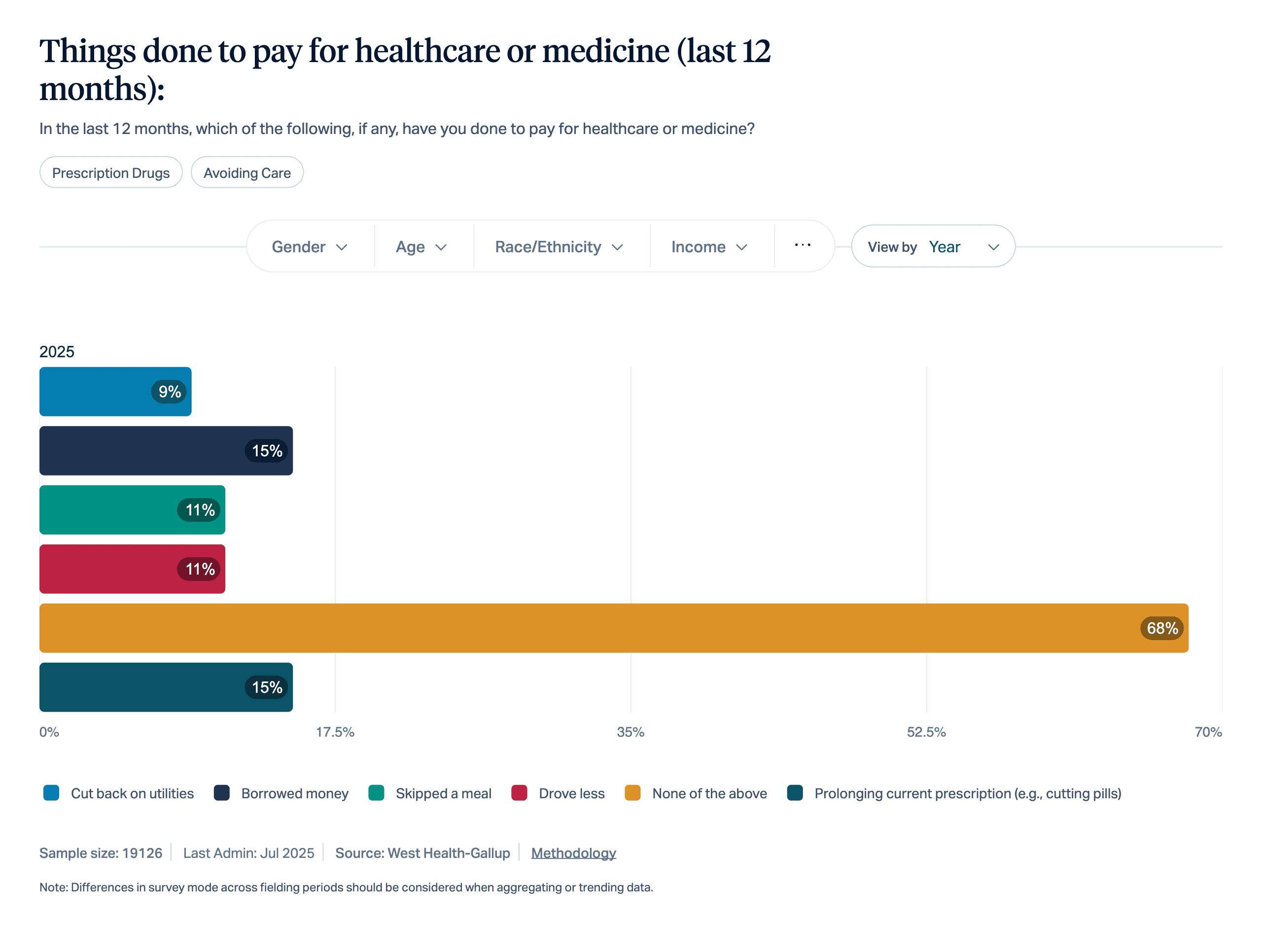
Food insecurity is largely related to economic and access factors. Many older adults live on a fixed income that is not keeping pace with rising costs of living, including groceries. They also face competing costs such as health care, prescription drugs, and housing costs that leave less money available for food, even among people not living in poverty. According to the Elder Index, up to 36% of older adults above the federal poverty level do not have enough income to meet their basic costs of living. Data shows that 19% of adults have had to sacrifice food in order to pay for health care. Findings from the West Health–Gallup Healthcare Affordability Index further highlight this tradeoff, with many adults reporting skipped or reduced meals due to medical costs. These data underscore how rising health care costs directly contribute to food insecurity by forcing households to make difficult tradeoffs between essential needs. Similarly, a report from New York State found that older adults diverted rent money, delayed or skipped utility payments, and relied on credit cards to purchase food.
Older adults living in food deserts or with transportation or mobility limitations also face barriers to healthy and affordable food. Because people in food deserts live far away from grocery stores, they often depend on convenience stores, gas stations, dollar stores, or food pantries, and these options typically lack healthy, affordable food. Even outside of food deserts, unreliable or inaccessible transportation and accessibility barriers within grocery stores contribute to food insecurity for older adults and people with disabilities.
These barriers contribute to certain populations of older adults experiencing higher levels of food insecurity than others. Socioeconomic disparities play a significant role: people eligible for both Medicaid and Medicare are at a higher risk of food insecurity and malnutrition-related complications than peers who are not eligible for both programs. Older adults of color experience food insecurity at disproportionately high rates — about one in five Black and Latino older adults experience food insecurity, compared to one in 16 white adults age 60 and older and one in 10 white adults age 50 to 59. Housing status also matters, as older adults who rent are more than three times as likely to experience food insecurity as those who own their homes.
Differences in access are especially clear when you look at the geographic concentration of food insecurity. According to Feeding America’s most recent Map the Meal Gap Report, 86% of counties with the highest rates of food insecurity (where 20% or more of the population experiences food insecurity) are in the South and are rural, despite only 45% of all U.S. counties being in the South and 62% of all counties being rural.
Food Insecurity and Malnutrition
Food insecurity is also closely tied with malnutrition. Today, one in two older adults is either at risk of malnutrition or is malnourished. Malnutrition is associated with increased morbidity and mortality and impacts of recovery from illness and surgery.
Rates of malnutrition is higher in older adults who are living in long-term care facilities (29%), rehab/subacute care facilities (29%), nursing facilities (17.5%), or hospitalized (22%), compared to older adults in the community (3%) and receiving home care services (9%). Quality and availability of food is a major contributing factor to malnutrition, which puts older adults experiencing food insecurity at greater risk.
However, older adults who are food secure can also be at risk of malnutrition due to a variety of other aging-related factors that affect food intake including changes in appetite, sensory abilities, oral health, cognitive health, side effects of illness and treatments, social isolation, and mental health.
Programs Addressing Food Insecurity for Older Adults
There are several federally funded programs that help alleviate food insecurity among the nation’s older adult population:
SNAP: Next to unemployment insurance, the Supplemental Nutrition Assistance Program (SNAP) is the most effective program addressing food insecurity in the country. This federally funded program, which is administered by states and/or counties, provides a monthly stipend to participants that can be used to purchase food at participating food stores and farmers' markets.
Medicaid: Older adults who qualify for Medicaid may receive food assistance through their state’s home- and community-based services program, in lieu of services, or nutrition-focused Medicaid 1115 waivers. As of 2024, 19 states offer some type of nutrition-related benefits under Medicaid waiver programs. This Center for Health Care Strategies brief outlines allowable nutrition-related Medicaid benefits for a range of food insecurity needs, including home-delivered meals, case management for access to food/nutrition, nutrition counseling, nutrition prescriptions tailored to health risk or health conditions, and grocery provisions.
Medicare: Though traditional Medicare does not provide nutrition benefits, older adults who are enrolled in a Medicare Advantage health plan may receive food assistance in the form of grocery allowances, which have been shown to increase rates of annual wellness, primary care, and specialist visits among some members, mitigating the health-related impacts of food insecurity.
Senior Nutrition Program: The Older Americans Act provides federal grants through the Senior Nutrition Program to states, territories, and tribal entities to support home-delivered and congregate meal programs for older adults facing significant economic or social needs, including those with low incomes, from low-income minority groups, living in rural areas, with limited English proficiency, or at risk of institutionalization. These programs are often administered by local governments or community-based organizations and funded partially or fully through these grants. Meals on Wheels, for example, is one of the most recognized home-delivered meal programs for older adults, and 89% of Meals on Wheels providers receive federal funding, including Older Americans Act funds. In addition to food, these programs provide older adults with opportunities for social connection, wellness checks, health education, and referrals to other needed supports and services.
USDA Programs: In addition to SNAP, the USDA funds several programs that serve older adults with food insecurity, including the Commodity Supplemental Food Program, Senior Farmers Market Nutrition Program, Child and Adult Care Food Program, and some locally-operated congregate and home-delivered meal programs.
While these programs assist a large share of older adults facing food insecurity, there are many older adults who either do not qualify for these programs or do not take advantage of their benefits for a variety of reasons, including stigma, low awareness, enrollment barriers, and immigration concerns. For example, after accounting for state income limits, an estimated 44% of people experiencing food insecurity may not be eligible for SNAP, and in 2022, nearly 60% of older adults who qualified for SNAP did not claim these benefits.
Many older adults in the “missing middle” similarly do not qualify for Medicaid programs but do not have enough income to cover the costs of health care or housing, and therefore need to make tradeoffs to afford food. One aspect of eligibility requirements for these means-tested federal programs is based on a federal measure of poverty that has not been updated since 1969 (except to adjust for inflation), and many experts agree it is no longer adequate to qualify people who need these programs. Reexamining eligibility criteria and adjusting programs to account for today’s rising costs of living is necessary to truly address food insecurity in our nation’s older adults.
