Executive Summary
The U.S. healthcare system faces a growing crisis: an aging population with increasing care demands amid severe workforce shortages. While adults age 65 and older currently make up less than a fifth of the population, they drive 36% of spending on healthcare—the highest of any age group. Furthermore, older adults are expected to outnumber children under the age of 18 for the first time in U.S. history by 2034, further widening the gap between patient needs and provider availability. The AAMC projects a shortage of up to 124,000 physicians by 2034, and a shortage of 27,000 geriatricians alone in 2025.3 Direct care faces similar challenges, with shortages expected to surpass 100,000 direct care professionals by 2030 and turnover rates exceeding 80%.
The growing disconnect between demand for older patient care and the shrinking healthcare workforce is made worse by pervasive ageism. Aging is often framed as something to resist or conceal, fostering both external bias and internalized shame. A University of Michigan poll found that 93% of older adults routinely experience ageist stereotypes, and 65% report regular exposure to media or messaging that suggest older adults are “unattractive or undesirable.” Even the projected increase in Americans 65 and older over the next ten years has been dubbed “the gray tsunami.” Beyond perception, ageism has tangible costs—the Yale School of Public Health estimates that ageism costs patients an additional $63 billion per year in healthcare spending.
“Of all the ‘-isms’ that are out there, one of the most ubiquitous and silent is ageism. We have very negative perspectives of aging. It’s all about decline, all the things you lose as you age. If we don’t address this, we are not tapping into the wisdom, the experience, the intergenerational opportunity, and better health.”
Dr. Charlotte S. Yeh, Former Chief Medical Officer, AARP
“The [clinician]-patient relationship is sacred. It’s eroding in large part because [clinicians] just don’t have the time.”
Dr. Andy Wagner, Chief Medical Officer, Affineon
Summary of Framework for Understanding Barriers and Opportunities in Older Patient Care
Societal attitudes toward aging affect both older adults’ ability to receive the care they need and the healthcare workforce’s ability to meet their needs. AI presents an opportunity to bridge this gap, enhancing both patient outcomes and provider capabilities. This can be understood across three levels of influence:
Societal Condition: Describes a set of circumstances that shape the experiences of individuals and groups within a society
Industry Implication: Potential effects that a societal condition might have on a group of individuals and/or organizations; in this case, healthcare
Opportunities for Impact: Strategic pathways for a solution (like AI) to transform challenges, repositioning them for growth and positive change
Image 1: Framework for Understanding Barriers and Opportunities in Older Patient Care
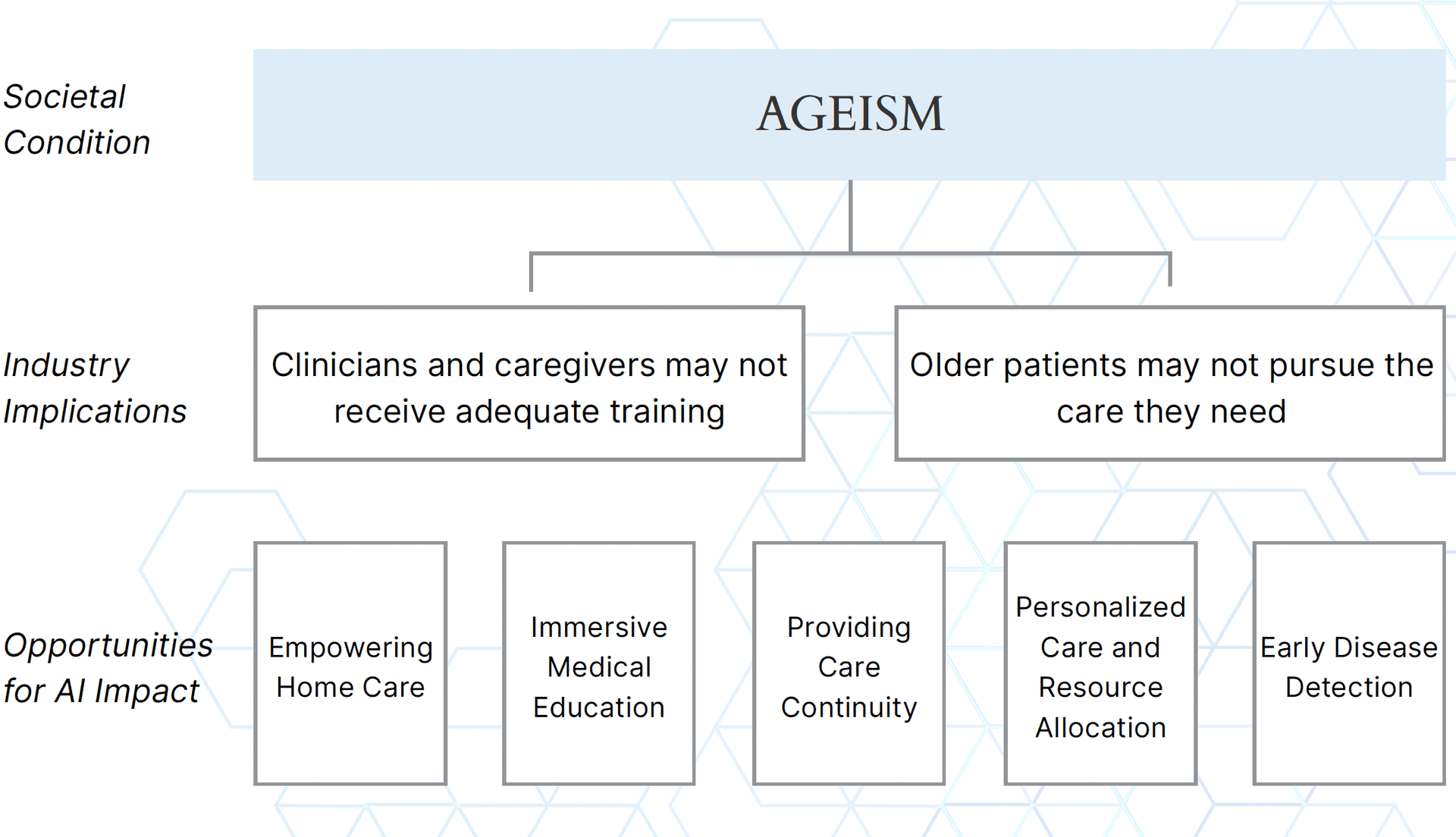
Industry Implications
Despite the wide variability in how people age, healthcare and society often fail to recognize these differences, instead viewing aging with discomfort and embarrassment. When ageism permeates healthcare delivery, it affects how healthcare workers provide care and how older patients seek it—often leading to unmet patient needs.
Implication for the Healthcare Workforce: Clinicians and caregivers may be prevented from providing appropriate care when they are trained to dismiss some health concerns as merely byproducts of aging rather than an conditions and diseases that should be managed or addressed.
Implication for Patients: Older patients may be hesitant to seek care for conditions typically associated with age because of the accompanying shame, potentially leading to more serious health concerns as these conditions are neglected
“The healthcare workforce is so often focused on fixing things. But aging is different, it’s about navigating a new way of life. Healthcare should be cradle to grave for everyone.”
Ramsey Alwin, President and CEO, The National Council on Aging
Opportunities for AI Impact
Technological innovation presents a critical opportunity to support the healthcare workforce amid growing shortages, while improving health outcomes for older patients. Artificial intelligence (AI) offers a versatile range of applications to address healthcare’s most pressing challenges, including more personalized and proactive care for older adults. AI will not replace the human connection that is integral to older patients’well-being, but will serve as a tool to better equip healthcare providers in meeting older patients’ unique needs. In doing so, AI can help alleviate the strain of workforce shortages and empower patients to confidently manage their health. This report highlights five key opportunities for AI to enhance the care of older adults:
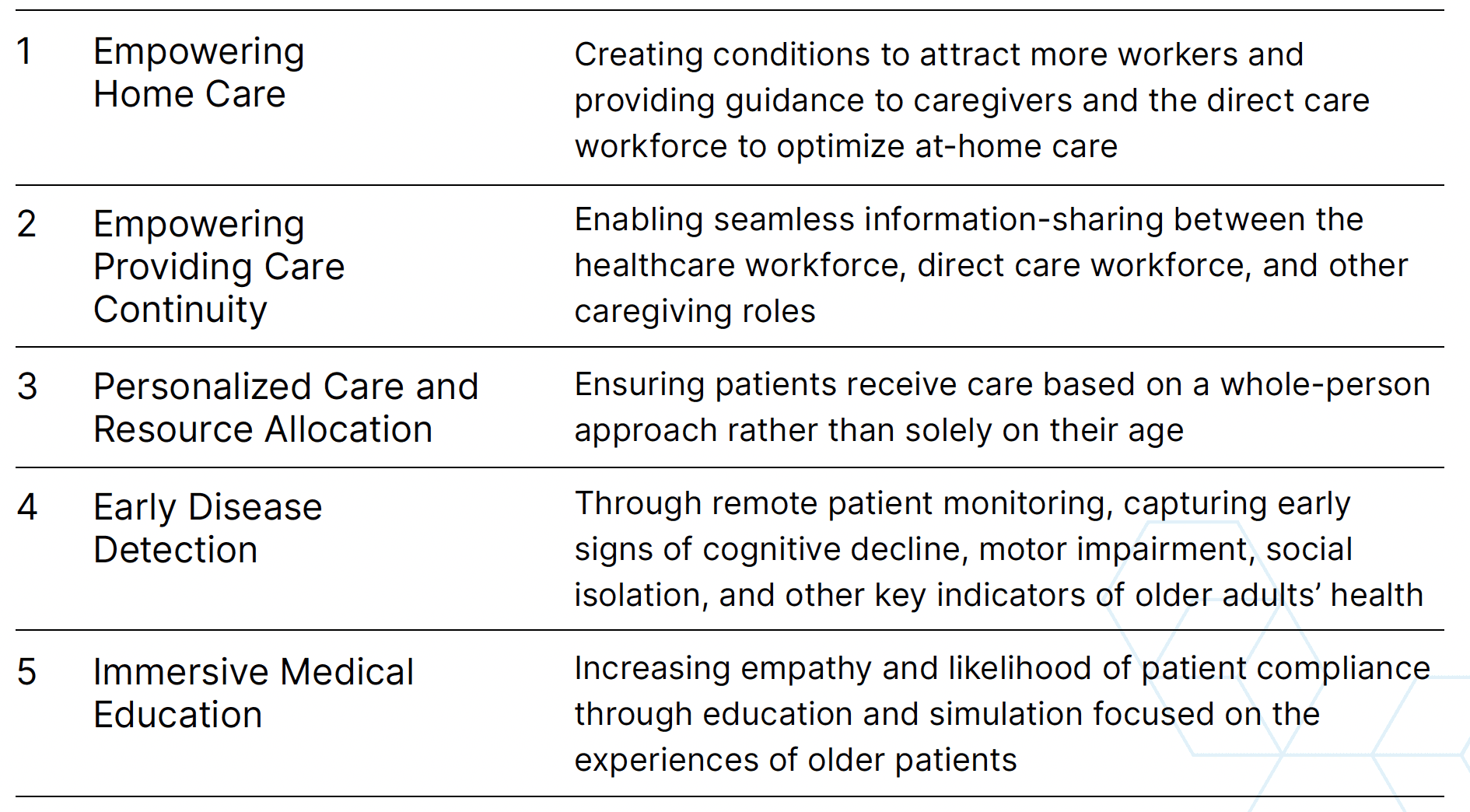
Additional Considerations
As described in this report’s predecessor, The Future of the Healthcare Workforce: Exploring How AI will Augment Delivery of Care in the United States, technology serving the healthcare ecosystem must account for the industry’s complexity, high level of regulation that often varies state by state, and need for interoperability. Beyond these considerations, two industry perspectives will expedite the effective use of AI tools in supporting healthcare for older patients:
Prioritization of gerontology-focused training and collaboration across specialties of healthcare for a range of healthcare and direct care providers
Willingness to innovate and invest in technology for the care of older patients
The applications of AI are rapidly changing, revealing a need for evaluation criteria that can remain relevant for future iterations of AI tools. To ensure the resilience of such tools, AI solutions that support the care of older adults should be developed according to the following criteria:
Decreases overall cost of care delivery for both patients and healthcare organizations
Capabilities are informed by the needs, wants, and experiences of clinicians and direct care professionals
Capabilities are informed by the needs, wants, and experiences of older adults
Introduction
American society is deeply anti-aging. Youth is idolized, while growing older is often framed as a problem to solve rather than a natural process. From skincare commercials to workplace culture, the message is clear: aging should be delayed, hidden, or fought against. Products promising to “reverse” aging flood the market, reinforcing the idea that looking young is the ultimate goal.
The media play a major role in shaping this negative perception of aging. Older characters in movies and TV shows are often portrayed as frail, forgetful, or out of touch.10 These portrayals reinforce the idea that aging is something to be feared rather than embraced, creating barriers for older individuals that make it harder for them to be seen as valuable contributors to society. Ageism also permeates healthcare, the effect of which is exacerbated by the fact that people over the age of 65 utilize care more than their younger peers.11 This bias has direct consequences:
Overlooked care: Older patients often struggle to get the care they need, whether it is because they hesitate to seek care for stigmatized conditions typically associated with age (e.g., hearing loss), or because healthcare providers may dismiss symptoms as consequences of aging rather than signs of a disease that should be treated.
Inadequate treatment: Focusing disproportionately on age prevents some healthcare professionals from providing the appropriate level of care to older patients. Often, they aren’t trained adequately for this patient population; healthcare providers may be operating under inaccurate assumptions about these patients’ abilities and goals that prevent them from offering comprehensive treatment options.
Lack of investment: More so than other patient cohorts, investment in care and technology for older adults is inadequate. While the number of older adults who own a smartphone rose from 18% in 2013 to 83% by 2021, and telehealth usage among older patients jumped from 4.6% to more than 21% following the COVID-19 pandemic, the industry continues to overlook this large and growing segment of the patient population.
“The reality is as all of us are living very non-linear, multi-stage lives today. We no longer spend a third of our years growing up and learning, a third of our years working and building a family, and a third of our years retiring and going off into the sunset and enjoying leisure. Instead, our education journey, our caregiving journey, and our work journey all have ebbs and flows.”
Ramsey Alwin, President and CEO, National Council on Aging
Societal Conditions and Industry Challenges
Against these headwinds, demand for healthcare services among older Americans is growing much faster than the available supply, with some 11,400 Americans turning 65 every day. As of 2022, there were 57.8 million people aged 65 or older in the U.S., representing 17.3% of the population. Older adults will continue to make up a larger proportion of patients across healthcare settings, exacerbating the existing strain on the healthcare workforce. Furthermore, the growing preference of older adults to age in their homes is similarly increasing pressure on the direct care workforce. A 2021 study by AARP found that 77% of adults over 50 would prefer to age at home; this preference aligns with the nationwide decrease in nursing home utilization. With such a large proportion of older adults planning to receive care in their homes, infrastructure to empower the healthcare workforce in meeting this demand will be critical.
Shortage of qualified home care staff: The U.S. home care workforce is facing a severe shortage, with serious implications for aging patients who need consistent and quality care. This shortage affects every level of the industry, from doctors and nurses who provide hospital-at-home, acute care, and post-acute care, to home health aides, making it harder for older adults to receive timely and reliable support. The gap between available care and the needs of older adults is widening, raising concerns about access, affordability, and overall quality of life for older adults. As a result, professional home care remains prohibitively expensive and Medicare supplemental plans and private insurance often provide limited coverage, forcing families to pay out of pocket.
Inconsistency of home care: Compounding the workforce shortage is the lack of standardization in the home care services available to older Americans. Unlike hospitals and medical clinics, which operate under strict regulations, home care services vary widely in quality, training requirements, and oversight. Some agencies provide well-trained aides and nurses, while others operate with minimal qualifications, potentially leading to inconsistent care and health outcomes.
Industry-wide retention challenges: Workforce shortages across the industry are further driven by deep-seated ageism in healthcare, limiting the attraction of new entrants to the field. Clinicians often receive minimal training specifically in geriatric care, while home care workers are frequently undervalued, underpaid, and overworked. Roles associated with the care of older patients, especially direct care, are not always positioned as highly-respected members of the care team, which can further discourage new professionals from entering the field.
Opportunities for Impact
In summary, the primary challenges in providing care to older patients include:
A workforce that needs specialized training
High cost of care delivery
Complex healthcare needs among patients
Rising demand due to an aging population
Technology plays a critical role to help address the challenges that older patients face when navigating today’s healthcare system, from artificial intelligence (AI) systems that automate common tasks to remote monitoring and predictive analytics that forecast disease and improve outcomes. These kinds of opportunities for AI to assist with providing care to this age demographic present an opportunity to improve efficiency and quality of care for older adults. However, to fully realize the potential of AI in this realm, it is crucial that these technologies are fully integrated into existing healthcare and direct care practices and that they are designed to work in tandem with, and support, human healthcare providers.
Use Case 1: Empowering Home Care
The home care industry is one of the fastest-growing segments of healthcare, with employment of home health and personal care aides projected to increase by 21% through 2033 according to the U.S. Bureau of Labor Statistics. That places direct care among the fastest-growing occupations in the country for the years ahead, driven by increasing demand from an aging population and a healthcare ecosystem unable to meet the needs of all patients in existing facilities. Home care has also been found to improve outcomes and reduce re-hospitalization rates, particularly for older individuals who may have limited mobility and struggle to travel to and from appointments.
While more and more patients prefer to remain at home as they age, there remains a shortage in the direct care workforce and varying levels of knowledge and training among these roles. By some estimates, there could be as many as 4.6 million unfilled positions for home health aides by 2032, with low pay, unpredictable work schedules, and limited career mobility commonly cited as reasons for the continued shortfall.17 Family members often assume the responsibility of caregiving for relatives, but they are rarely formally trained and often attempt to navigate these responsibilities from a distance or while juggling other work and family obligations.
Description
AI can augment traditional home care by improving efficiency and enhancing the quality of patient support. By automating administrative tasks such as scheduling, it reduces the time and effort required for manual coordination, lowering overhead costs and allowing direct care to focus more on patient care. Additionally, AI can synthesize data from disparate sources—such as medical records, real-time health monitoring devices, and caregiver notes—to create a comprehensive and unified profile of a patient. This holistic view enables home care workers to deliver more consistent, high-quality care and helps family members stay informed and actively involved in managing their loved one’s well-being.
Key Benefits
Cost savings: AI can decrease overhead and training costs for home health providers, potentially reducing the cost burden on older clients living on fixed income and allowing caregivers to be paid higher wages for their work.
Provider retention: According to the Home Care Association of America, median turnover in the industry increased to 79.2% in 2023, highlighting the need to attract qualified, professional caregivers and retain them over time. Ease of service delivery using AI and the potential for higher pay could both make the field more attractive to workers and encourage those already in the field to stay.
Improved patient outcomes: By reducing variability in care arrangements and enabling real-time adjustments for a patient’s care team, AI can help improve overall patient outcomes while in home care and reduce the need for additional hospitalization or inoffice follow ups.
Key Consideration
Process integration: AI-powered home care systems will need to seamlessly integrate with providers’ existing and future databases, like the electronic health record (EHR), for care management and tracking. The interfaces themselves must also be user-friendly and accessible to all home health aides, regardless of their tech familiarity, in order to ensure consistent use and application in the field.
Patient buy-in: Some patients may be unfamiliar with the AI tools available to healthcare providers today and many remain skeptical of their use in their care, with 74% saying they have “very little or no trust” in online health information that they know was generated by AI. It could take time for these patients to adjust to the use of AI in their care; providers should consider slowly rolling out services as needed to allow end users to become more comfortable with this technology over time.
Balancing Efficiency with Care: While it’s crucial that home care and healthcare generally find ways to be more efficient through the use of AI and technology, ethical considerations demand careful implementation to ensure high quality of care and strong human connections.

Use Case 2: Care Continuity
Supporting the future healthcare workforce will require bridging the gap between the institutional healthcare workforce, the direct care workforce, and other caregiver roles. Without alignment and communication among different members of a patient’s care team, healthcare providers are left with incomplete information that can lead to redundant care, unnecessary tests, and inefficient management of comorbidities. Overall, care suffers and patient outcomes decline as a result; a 2018 study found an association between strong continuity of care and reduced all-cause mortality, and another in 2023 found a link between fragmented care and poor outcomes for patients with chronic illnesses.
Such communication barriers typically arise at transitions between different sites of care. Despite the best efforts of all involved, information and treatment plan details can be lost between the hospital, post-acute care, and home. These challenges have only been exacerbated by the ongoing loss of primary care providers, changes in health insurance care requirements, and the rise of remote care and telehealth services.
Description
AI can help ensure care plans, medication compliance, and other dimensions of care are tracked and preserved across providers, no matter where they are physically located. Technology can enable critical coordination in bringing the different members of a patient’s care team together, ordering services, tracking progress, and updating treatment plans. Automating care continuity activities further lifts the burden of communication from the healthcare and direct care workforces, allowing them to focus more of their time on direct patient care.
Key Benefits
Personalized treatment plans leveraging predictive analytics: By analyzing community outcomes data and using it to tailor treatment plans that are specific to each patient, AI can help ensure care continuity across different providers and care settings. Layering in predictive analytics in this way has been shown to improve patient outcomes and deliver better care at scale, allowing for proactive intervention and smoother care transitions.
Automated documentation: Miscommunication is at the core of many care continuity challenges, but AI-powered systems that automate care documentation and note sharing, like ambient AI scribes, can ensure that all involved in the patient’s care have access to the same information and know the current state of treatment at all times.
Key Considerations
Data privacy and security: Data security and cyber protections must be in place to ensure clean data for care team use and foster trust that the system is giving them the accurate information they need to make decisions. Further, HIPAA regulations protect patient information and must be integrated into any AI care continuity system.
Interoperability: Any AI used for continuity of care must provide a strategy to integrate with existing EHR systems. Such considerations help avoid data silos and ensure smooth information flow between providers, facilities, and other care team members. Interoperability of AI-enabled care continuity also helps transfer the responsibility of information verification and coordination from healthcare and direct care teams to the AI Tool.

Use Case 3: Personalized Care and Resource Allocation
When cultural conditions of ageism permeate healthcare, age can become a primary determinant of care for older patients. Treatment decisions may then be made based disproportionately on age-related factors rather than a whole-person view of the patient’s unique circumstances. In these cases, other critical determinants of health may slip through the cracks when they are viewed simply as a byproduct of aging rather than a more serious condition that requires a modified care plan. One example is hearing loss, which is common in many older adults but may also lead to cognitive decline if left untreated.
But aging is a spectrum; older patients may not be considered for more ambitious care such as surgeries or experimental treatments because of their age, even if they are active, healthy, and otherwise good candidates. In fact, some 20% of patients over 50 have faced age-based discrimination in their healthcare. Left unaddressed, these oversights can contribute to additional complications for patients including long-term cognitive decline, increased time in the hospital, reduced quality of life, depression, and more. A recent McKinsey survey on health outcomes found that 33% of respondents reported unplanned and costly follow-up care as a result of these types of preventable causes. Without the assistance of technologies like AI, providing the level of personalized care that is needed to address these concerns may be more resource-intensive than the current healthcare system can accommodate—often in terms of human resources, bed space, and cost.
Description
AI can help bridge this gap by developing personalized care plans for older patients based on a comprehensive profile, including their lifestyle and activity level, that accurately reflects their true, whole-body condition and goals rather than just their age, thereby leveling the playing field and reducing age discrimination. Further, AI can also be used to assess overall risk and acuity levels to determine what level of care is appropriate and when it will be most effective. For instance, this type of personalized data might be used by physicians to determine the right cadence and frequency of physical therapy appointments following joint replacement surgery based on each patient’s individual health situation.
Key Benefits
Optimized treatment plans: Rather than relying solely on community standards, AI-driven personalized treatment plans can be optimized to each patient’s unique health needs and circumstances. Many patients perceive these personalized care plans as more effective, and 72% say they want access to more personalized care as a result.
Tailored medications and therapy: AI can help adjust medication dosages and prescriptions based on a patient’s genetics, lifestyle, and health history. Personalized rehabilitation and therapy schedules can lead to improved recovery outcomes and reduced readmission rates.
Cost savings: By reducing complications and the risk of related developments (such as cognitive decline in patients experiencing hearing loss), AI optimization can provide new cost savings for patients and providers through its enablement of more effective preventative care, helping older patients effectively identify and address current health concerns and avoid more serious conditions. Downstream, this approach refocuses the healthcare workforce onto higher-need cases. In this way, AI can help ensure that healthcare resources are used where they are most needed.
Key Considerations
Data privacy: Given that AI will rely on patient data to inform personalized healthcare support, sharing sensitive patient health data with these systems means that data privacy will be critical to foster trust with patients and clinicians.
Comprehensive Trainings: Particularly in the early use of this technology, there is a possibility for error in AI results when models are not trained on patient populations that reflect the patients to whom they are providing personalized guidance. To mitigate this concern, AI tools that support personalized care for older adults should be trained on patient data that includes a broad range of conditions, lifestyles, and activity levels.

Use Case 4: Early Disease Detection
Early disease detection has long been shown to improve patient outcomes and decrease the need for invasive treatments. In breast cancers, for instance, cases that are caught in their earliest, localized stages have a five-year survival rate of 99%.28 Early detection is particularly important for older patients, as disease progression can mean the difference between a manageable condition and invasive required treatments that have a long-term negative impact on the patient’s quality of life. Primary care is typically the focus of most early detection efforts for patients of all ages, but the early signs of cognitive decline, physical disability, or social isolation may be written off as signs of aging. If found early, these key determinants of health can be addressed before symptoms advance.
Description
AI can enable remote patient monitoring through wearables, fall detection, and other technologies that may be trained to recognize early signs of decline or disease—and recommend a course of action.29 Beyond simple monitoring, however, AI can also increase the efficacy of these existing wearable technologies by enabling more sophisticated data analysis and predictive modeling capabilities. In this way, patient monitoring systems can be used as early disease detectors, proactively watching for symptoms and raising alerts when patients begin showing signs of more severe decline before they are seen by a clinician.
Key Benefits
Leveraging predictive analytics: As with traditional diagnostics, data collection is just one part of the process. Identifying connections and trends in that data is required to uncover the full picture of a patient’s health. AI can enable predictive insight into health data in real time, leading to the potential for faster disease detection and more timely alerts to potential complications. AI can also identify risk factors and warn about potential health concerns before symptoms appear.
Increased accuracy at scale: Advanced algorithms can potentially reduce misdiagnoses by spotting subtle patterns in scans and tests before the patient’s care team does.
Less invasive for patients: By monitoring at home through tools such as biomarkers, imaging, and wearable devices, AI can help providers detect diseases without the need for invasive testing procedures. Early intervention can also help prevent emergency visits and future hospital stays.
Key Considerations
Data quality: AI tools are not positioned to make healthcare decisions in a vacuum. Clinicians should be prepared to review patient data when AI systems are used for early detection to ensure its findings are correct, identify additional areas for intervention, and address conditions that have been detected.
Regulatory concerns: While remote patient monitoring is well-established, the addition of AI-powered tools that make use of that monitoring data could potentially contribute to new privacy concerns for regulators. Regulatory changes and additions could limit the applicability of AI systems targeting early detection.

Use Case 5: Immersive Medical Education
Traditional medical training emphasizes clinical knowledge but may sometimes overlook the lived experiences of older patients. Understanding age-related challenges—such as mobility issues, sensory impairments, and day-to-day difficulties—often requires perspectives beyond the medical textbook. Without first-person experience of what aging feels like and what it means to live in an older body, it may be difficult to fully grasp the effect of things like difficulty walking, reduced grip strength, or hearing and vision loss—and design optimized care plans for those differences in ability.
Education and simulation-based training can bridge this gap, allowing healthcare providers to step into the shoes of their older patients. By experiencing what it is like to navigate the world through the lens of an older patient, clinicians can tailor care accordingly.
When clinicians don’t have access to the perspectives of older patients, this potential disconnect and lack of understanding can lead to frustration from both the clinician and the patient. A member of the care team may recommend a treatment plan that seems straightforward—like taking multiple medications at different times of the day—without considering dexterity issues or cognitive changes that make adherence difficult. Conversely, they may underestimate an older patient’s capabilities, discouraging physical activity or independent decision-making when the patient is still capable of maintaining autonomy. Such misjudgments can negatively impact both health outcomes and patient-provider trust.
By integrating experiential learning into training programs, healthcare professionals can refine their approach to care for older adults. When providers truly understand the unique barriers older patients face, they can design care strategies that are both effective and practical—ultimately improving compliance, fostering trust, and enhancing overall quality of life.
Description
AI-enabled Virtual Reality (VR) and Augmented Reality (AR) simulations can immerse clinicians in the daily challenges faced by older patients, including mobility limitations to cognitive impairments, enabling more realistic scenario training in care for older adults. These technologies replicate real-life conditions like vision loss, arthritis, or dementia, helping healthcare providers understand and empathize with the physical and emotional impact of aging. AI and VR/AR technologies also have the potential to scale up clinical training efforts specific to the care of older adults, thereby helping the industry meet the care needs of the growing population of older patients.
Key Benefits
More realistic scenario training: AI and VR/AR technology can create lifelike simulations of older patients with diverse medical conditions, allowing clinicians to practice diagnosing and treating age-related conditions in a risk-free virtual environment. By experiencing these challenges firsthand, clinicians can empathetically adjust their approach to care, whether through adjusted communication, modified treatment plans, or more patient-centered solutions.
Improved communication skills: Using AI and VR to simulate sensory impairments like hearing loss and arthritis can help providers better understand the day-to-day challenges that patients are facing and hone their communication skills to work with patients facing these types of conditions.
Standardization in training: AI can ensure consistent education for practitioners across different locations and skill levels, improving overall care quality and helping the industry keep pace with growing workforce demand.
Cost effectiveness: AI, VR, and augmented reality (AR) educational tools are relatively inexpensive, high-impact ways to deliver medical education outside of a traditional classroom environment. As these resources become more widely available, access to AI, VR, and AR enablement can help reduce the already-high cost of clinical training and education while also providing realistic scenario training.
Key Considerations
Education Support: While barriers to access for AI-enabled immersive education should be addressed, leaders must also consider additional education needs associated with AIenabled tools. AI lessons and VR interfaces should be bolstered with introductory training on these new learning tools to preserve their efficacy.
Lack of emotional nuance: Healthcare is deeply human and calls for a full appreciation of human emotions and attitudes that cannot be replaced or replicated by AI. Practitioners trained using AI and VR systems should maintain access to real-world clinical experiences as a part of their education.

Conditions for Success
The healthcare and direct care workforces who provide care to older patients operate in an industry that is historically slower to prioritize and adopt new technologies, but there are clear opportunities for AI to bridge the gap between patients’ needs and the workforce’s capabilities. As outlined in this report’s prerequisite, The Future of the Healthcare Workforce: Exploring How AI will Augment Delivery of Care in the United States, the broader impact of AI across healthcare can be fully realized only when key conditions are met by both the market and regulatory authorities.
Reliable, transparent, and auditable models: Trust from patients and clinicians is paramount to the success of AI in this space, where transparency and traceability build confidence in the guidance provided by AI tools.
Industry-wide adoption: AI’s success depends on buy-in from healthcare organizations, clinicians, non-clinical staff, and patients. Aligned incentives—cost savings, efficiency, and better care—will drive engagement. Regulatory incentives may also play a role.
Unified regulations: State-by-state differences in laws could slow AI’s impact. Streamlined regulations are needed to support AI-driven telemedicine and at-home care.
Interoperability: AI must integrate seamlessly with existing systems, EHRs, devices, and care settings. Beyond these stakeholders, commercial insurers need to be included in the conversation.
Integration with medical education: Clinicians need AI training, as do all participants in the healthcare value chain. AI can also personalize learning, provide customized scenario training, and help ensure that practitioners stay up to date with evolving technologies and treatment demands.
Beyond these conditions that strengthen the opportunity for AI to support the healthcare workforce as a whole, there are additional considerations that are unique to the care of older adults. First, geriatric and gerontologic training and collaboration across specialties of healthcare can help this workforce better meet the unique needs of older patient populations through technology solutions. Additionally, there must be a shift in priorities for technology adoption in older patient care as well as a willingness to adopt and invest in innovative technologies that serve older patients to help meet the level and nature of their needs.
Cross-Specialization Involvement
By 2050, it is estimated that people 65 and over will represent over 20% of the U.S. population, up from barely 16% as of 2020. That population will need robust access to healthcare, but workforce shortages across the industry leave roles focused on older patient care at a disadvantage in meeting this incoming demand. There are currently only 7,500 geriatricians, or specialists in the care of older adults, in the U.S., but the aging population will need more than 30,000 to have their care needs met in the years ahead. Shrinking numbers of geriatric specialists reveal a need to ensure critical healthcare specialties, especially primary care, are provided opportunities to improve care delivery for older patients—thereby reducing bias and improving health outcomes. Clinicians across specialities will inevitably see more older adults as this patient population grows. When geriatric and gerontologic perspectives and training are extended across specialties of healthcare, clinicians are better equipped to optimize care in the context of their older patients.
Technology Investment
Despite the increasing demand for senior care, technology in this space often lags behind, forcing providers to rely on outdated systems. As the 65+ population continues to expand and workforce shortages intensify, the role of technology will become even more critical in ensuring high-quality, accessible care. AI-driven tools, remote monitoring systems, and automation can help alleviate staffing pressures, enhance efficiency, and improve patient outcomes. However, without a proactive and structured approach to integrating these advanced solutions, the healthcare system risks being overwhelmed by the rising number of aging patients who require specialized and continuous care. Highlighting the opportunity for innovation within this space—and the associated financial benefit for patients, health systems, and technology providers—can help reposition older patient care as an area ripe for investment.
Criteria for Supporting Older Patient Care with AI
The applications of AI are constantly shifting, and opportunities for AI to optimize care for older patients will likely extend beyond the use cases outlined in this report. When industry leaders seek to identify AI-enabled solutions that will strengthen the healthcare and direct care workforces’ ability to care for their older patients, three areas of inquiry can help inform such assessments.
Decreases overall cost of care delivery
When AI-enabled technologies can streamline operational inefficiencies and help reduce non-clinical expenditures within the care delivery process, resources can be strategically reallocated to increase direct compensation for clinicians. This improved reimbursement will serve to elevate the attractiveness of geriatric and gerontologic care professions, thereby strengthening workforce recruitment and retention. Additionally, evidence of reduced costs associated with care delivery helps encourage adoption and investment in innovation for older patient care. If healthcare and direct care organizations are provided evidence of clear return on technology investments, they are more willing to embed such technologies in the delivery of care.
What to look for
Demonstrable cost analysis: Has the ability to identify and measure differences in key performance indicators within care delivery, like cost, to quantify the efficacy of the tool.
Developed according to insight from clinicians
Technology innovation must be informed by the clinicians who will use it to inspire adoption and build trust in the systems themselves. Involving healthcare professionals in the development process ensures that any AI application aligns with their workflows, addresses their challenges, and is intuitive enough for seamless integration with existing medical practices. Only with this buy-in can providers effectively communicate the value of AI to their patients.
What to look for
Inclusive development: Built with diverse input from clinicians and practitioners across care settings and geographic areas in order to include feedback from multiple specialties.
Data transparency: High-quality, reliable source data that can be tracked and verified when used in clinical settings.
Developed according to insight from older patient demographics
Technology innovation in healthcare must be guided by the voices and experiences of the patients it aims to serve. Without their input, even the most advanced solutions risk missing the mark on real-world needs, leading to inefficiencies or lack of adoption. Engaging patients early and often helps ensure that new technologies are not only practical but also build trust, fostering a sense of collaboration rather than imposition.
What to look for
Designed with patient input: By prioritizing patient perspectives, healthcare innovators can create AI-powered solutions that truly enhance care and improve outcomes without alienating those they are meant to serve. The development AI tools to support older patient care should include embedded frameworks to capture and implement the perspectives of older patients. Such frameworks may include comprehensive user testing and market research.
Ongoing iteration and improvement: AI development is not static, but an ongoing process of evolution and adaptation. In order to remain relevant to the older patient population, systems need to be constantly improving with an eye toward better patient adoption and outcomes.
References
McGough, M., Claxton, G., Amin, K., Cox, C. (4 January 2024). How do health expenditures vary across the population? Peterson-KFF. https://www.healthsystemtracker.org/chart-collection/health-expenditures-vary-across-population/
America Counts. (10 December 2019). 2020 Census Will Help Policymakers Prepare for the Incoming Wave of Aging Boomers. U.S. Census Bureau. https://www.census.gov/library/stories/2019/12/by-2030-all-baby-boomers-will-be-age-65-or-older.html
Boyle, P. (4 November 2021). Prescription for America’s elder boom: Every doctor learns geriatrics. AAMC. https://www.aamc.org/news/prescription-america-s-elder-boom-every-doctor-learns-geriatrics
Scales, K., McCall, S. (2025). Understanding the Direct Care Workforce. PHI. https://www.phinational.org/policy-research/key-facts-faq/
World Health Organization. (18 March 2021). Ageing: Ageism. https://www.who.int/news-room/questions-and-answers/item/ageing-ageism
DeAngelis, T. (1 September 2022). By the numbers: Older adults report high levels of ageism. American Psychological Association. https://www.apa.org/monitor/2022/09/older-adults-ageism
America Counts. (10 December 2019). 2020 Census Will Help Policymakers Prepare for the Incoming Wave of Aging Boomers. U.S. Census Bureau. https://www.census.gov/library/stories/2019/12/by-2030-all-baby-boomers-will-be-age-65-or-older.html
Allen, K. (13 November 2018). Ageism May Add Billions to Health Costs. AARP. https://www.aarp.org/health/healthcare/ageism-health-cost/
Martin, R. (18 October 2022). America’s obsession with staying young. Michigan Daily. https://www.michigandaily.com/statement/americas-obsession-with-staying-young/
Wangler, J., Jansky, M. (13 April 2023). Media portrayal of old age and its effects on attitudes in older people: findings from a series of studies. Nature. https://www.nature.com/articles/s41599-023-01671-5
Zayas, C., et al. (15 July 2016). Examining Healthcare Utilization Patterns of Elderly Middle-Aged Adults in the United States. Proceedings of the International Florida Artificial Intelligence Research Society Conference 2016. https://pmc.ncbi.nlm.nih.gov/articles/PMC4946167/
Mace, R., Matos, M., Vranceaunu, A. (8 September 2022). Older adults can use technology: why healthcare professionals must overcome ageism in digital health. National Institutes of Health. https://pmc.ncbi.nlm.nih.gov/articles/PMC9494377/
Administration for Community Living. (May 2024). 2023 Profile of Older Americans. https://acl.gov/sites/default/files/Profile%20of%20OA/ACL-ProfileOlderAmericans2023_508.pdf
Ratnayake, M., LPCMH, ATR, NCC; Lukas, S., Brathwaite, S., Neave, J., Henry, H., & BS-c;5 (2022). Aging in Place: Are We Prepared? Delaware Journal of Public Health, 8(3), 28–31. https://doi.org/10.32481/djph.2022.08.007
Goda, G., Van Houtven, C. (28 October 2024). Expanding in-home care coverage is a needed evolution of Medicare. Brookings. https://www.brookings.edu/articles/expanding-in-home-care-coverage-is-a-needed-evolution-of-medicare/
U.S. Bureau of Labor Statistics. (2024, August 29). Occupational Outlook Handbook: Home Health and Personal Care Aides. https://www.bls.gov/ooh/healthcare/home-health-aides-and-personal-care-aides.htm
O’Dell, M., Wheeler, L. (November 2012). Home Health Care: Healing Where the Heart Is. Missouri Medicine. https://pmc.ncbi.nlm.nih.gov/articles/PMC6179605/
Seeger, L. (16 October 2024). Could Worker Cooperatives be a Fix for the Home Care Worker Shortage? Harvard Public Health. https://harvardpublichealth.org/policy-practice/us-direct-care-worker-demand-outstrips-supply-can-co-ops-help/
Gavin, K. (16 October 2024). Misinformation, AI & Health: Poll Reveals Older Adults’ Worries. Michigan Medicine. https://www.michiganmedicine.org/health-lab/misinformation-ai-health-poll-reveals-older-adults-worries
Battista, M. (7 April 2024). Continuity of Care: How to Retain Patients and Reduce Redundancy. Creyos. https://creyos.com/blog/continuity-of-care
Joo, J. (9 January 2023). Fragmented care and chronic illness patient outcomes: A systematic review. Nursing Open. https://onlinelibrary.wiley.com/doi/10.1002/nop2.1607
American Medical Association. (25 October 2023). AMA president sounds alarm on national physician shortage. https://www.ama-assn.org/press-center/press-releases/ama-president-sounds-alarm-national-physician-shortage
Clack, L. (20 June 2023). Using Data Analytics to Predict Outcomes in Healthcare. Journal of AHIMA. https://journal.ahima.org/page/using-data-analytics-to-predict-outcomes-in-healthcare
Johns Hopkins Medicine. (2025). The Hidden Risks of Hearing Loss. https://www.hopkinsmedicine.org/health/wellness-and-prevention/the-hidden-risks-of-hearing-loss
Pelham, V. (16 October 2023). Confronting Ageism in Healthcare. Cedars-Sinai. https://www.cedars-sinai.org/blog/confronting-ageism-in-healthcare.html
Bestesny, O., Cordina, J. (5 August 2021). The role of personalization in the care journey: An example of patient engagement to reduce readmissions. McKinsey. https://www.mckinsey.com/industries/healthcare/our-insights/the-role-of-personalization-in-the-care-journey-an-example-of-patient-engagement-to-reduce-readmissions
Abbott. (19 August 2020). New Research Finds Physicians and Patients Point to Emerging Technology and Data as Central to Closing Treatment Gaps and Improving Vascular Health. https://abbott.mediaroom.com/2020-08-19-New-Research-Finds-Physicians-and-Patients-Point-to-Emerging-Technology-and-Data-as-Central-to-Closing-Treatment-Gaps-and-Improving-Vascular-Health
National Breast Cancer Foundation, Inc. (5 March 2025). Breast Cancer Facts & Stats. https://www.nationalbreastcancer.org/breast-cancer-facts/
Yuen, C. (17 February 2025). How is AI Used in Elderly Care Enhancing Lives and Support Systems. SNF Metrics. https://snfmetrics.com/ai-in-elderly-care
Gomstyn, A. (30 September 2024). Exploring privacy issues in the age of AI. IBM. https://www.ibm.com/think/insights/ai-privacy
Aquilina, T., et al. (24 January 2018). Springer. The involvement of older inpatients in medical student education. https://pmc.ncbi.nlm.nih.gov/articles/PMC5797205/
AARP International. (2025). United States. AARP. https://www.aarpinternational.org/initiatives/aging-readiness-competitiveness-arc/united-states
UNC School of Medicine. (18 August 2023). Aging America: The Growing Need for Geriatricians. https://www.med.unc.edu/medicine/news/aging-america-the-growing-need-for-geriatrics/

